SUMMARY
In the last ten years the treatment of lumbar disk herniation is significantly diversified. Other pathologies of the posterior vertebral compartment, as facet joint arthrits and spinal canal stenosis can complicate clinical symptoms. Because of this complex clinical syndrome the ozonetherapy found many applications, for its poor invasivity and low cost. Our clinical series of 96 patients, homogeneous for lumbar disk pathologies, age and sex, was divided in two treatment groups:
GROUP A treated with 12 injections of O2-O3 gaseous mixture in paravertebral muscles
GROUP B treated with 12 injections of only medical oxygen.
A reduction of subjective and objective parameters was observed in both groups. Excellent or good and fair results were observed in 86% of patients. On the other hand from our study arises a statistical evidence of a difference in evolution (time and intensity) of some clinical parameters between the two treated groups.
KEY WORDS:
INTRODUCTION
In the last ten-year period the treatment of lumbar disk herniation is significantly diversified, concerning the various surgical approaches more or less invasive (from the standard techniques to the percutaneous approaches, in which suction, laser or arthroscopic techniques have been advocated). Each of these methods demonstrates to have precise indications and a discrete incidence of failure. [11, 15]
Anyway the principal goal of these surgical interventions is the one of removal of the disk material already been extruded or still contained. Besides, in the cases in which the low back pain or sciatic pain is determined by recurrence of the disk protrusion or more simply by the scar tissue, which often involves the nervous root, even after some time past from the surgical intervention, the techniques above mentioned do not find very often any indication, and the alternative can only be an open surgical revision.[4, 7, 11, 12]
It is also important to underline how other pathologies of the posterior vertebral compartment, facet joint arthritis and spinal canal stenosis,[6, 10, 12, 14] can complicate clinical symptoms, which just for a small part are sustained by the real disk pathology. Because of this various and complex clinical syndrome the ozonetherapy found many applications, and that's for its poor invasivity, the absence of secondary effects and for the low cost.[1, 9, 13]
There is still to be clarified how some of the mechanisms, with which a mixture of oxygen and ozone acts on the nerve root involvement. In reality the success obtained with the introduction of the gaseous mixture lets us think of a direct effect of the ozone on the structural components of the intervertebral pulpous nucleus as collagen proteoglicans and water. Regarding this, there are many hypotheses, even if at the moment the anatomicopathological findings in man of how the gaseous mixture acted on the disk tissue are still poor. Actually, the biochemical events induced by the medical ozone on pulpous nucleus tissue, can be postulated by the chemical bond between ozone and water, giving arise to a " fall" of oxidant composites (Reactive Oxygen Species). These acting towards various substrates (glucose, galactose, N-acetil-glucosamine, glucuronic acid and glicine) determinate the break down of the glycosaminoglycans aggregates, leading to a collapse of their three-dimensional structure.[5] The R. O. S., diffusing itself, is able to act both on the extruded disk material and on the simple disk protrusion, leading to a decompression of the nervous root.[8]
There is also the hypothesis of an anti-inflammatory and local analgesic action, related likely to the ozone proprieties to modify the microcircle and the haemoglobin reduction mechanism, with consequent mayor release of oxygen to the tissues.[2]
Aim of our research is to find the main objective parameters (clinical and/or instrumental) that could at least make clear, as much as possible, the natural history of sciatic pain treated with medical ozone.
MATERIALS AND METHODS
The same group of three researchers has carried out this research in an Italian hospital (Department of Orthopaedic Clinic of Milan University) from January 1997 to June 1998.
96 patients, ageing between 19-85 years, of which 54 men and 42 women, affected by lumbar back pain and sciatica in presence of different lumbar spine disk abnormalities (disk protrusions, contained herniations, extruded herniations, relapses of disk herniations), in some cases joined with asimptomatic spinal canal stenosis or facet joints arthritis, underwent the oxygen-ozonetherapy by a cycle of lumbar muscles injections.[3]
Clinical evaluation has been confirmed by C. A. T. and/or M. R. I..
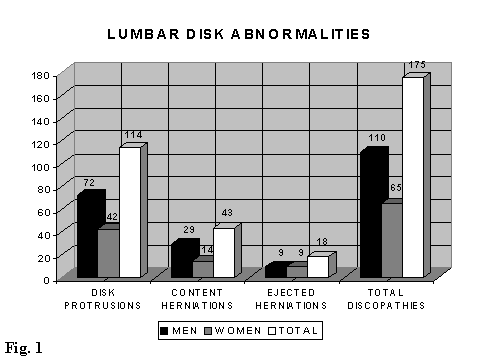
We found totally 175 disk abnormalities (110 in men and 65 in women) of which 114 disk protrusions (72 in men and 42 in women), 43 contained disk herniations (29 in men and 14 in women) and 18 extruded disks (9 in men and 9 in women) (Fig. 1).

Concerning this 96 patients, 20 (12 men and 8 women) were affected by relapse of slipped disk after previous surgery and 15 (9 men and 6 women) presented asymptomatic spinal canal stenosis.
All the patients reported in advance a pharmacological and physical treatment, without obtaining significant results.
The patients included in this study underwent the treatment according to the protocol S. I. O. O. T. 933902 with twelve local injections of an oxygen-ozone gaseous mixture, of which, eight, twice a week and the last four once a week for a total lasting of eight weeks. For each treatment session two single bilateral injections in the paravertebral muscles at the level of the discopathy were performed. In our series the gaseous mixture (concentration of ozone equal to 20 mcg/ml of oxygen) has been produced and sucked (by syringe of 20 cc) directly from the generator of O2-O3: with photometric system. On a prone patient, previous skin cleaning, 15 cc of medical ozone mixture have been injected at a distance of 2 centimetres from spinous processes in the paravertebral muscles with a needle of 21 G. Once reached the lamina, by needle tip, we draw back the needle just 2 or 3 millimetres, making sure not to be inside a blood vessel, and starting to introduce very slowly the gaseous mixture. After the two infiltrations was applied a piece of sticking plaster and than the patient was left on the couch for about 10 to 15 minutes time.
Our clinical series, homogeneous for lumbar disk pathology, age and sex, has to be divided into two groups regarding the type of treatment:
RESULTS
The global evaluation of the results permitted us to observe how the reduction of the subjective symptomatology has been shown both in the group A and B, with rhythms and times practically superimposable in every patient. The reduction of 20% of clinical signs was observed between the IV and the VI treatment session, of 60% between the VIII and the X session and of 90% at the end of the treatment (XII session).
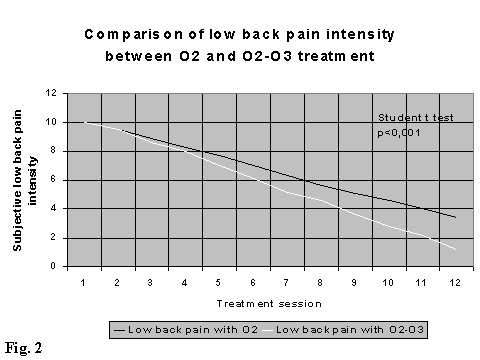
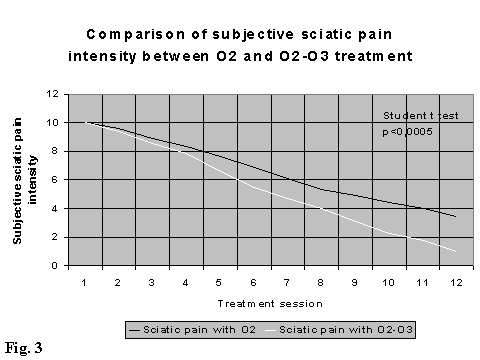
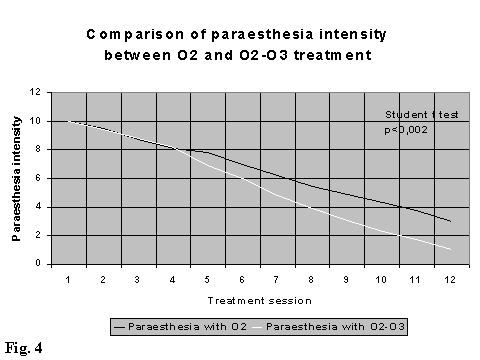
The control group B (treated with medical oxygen only) has shown a delay of about two weeks in comparison with group A (treated with medical ozone) in giving evidence of the reduction of clinical signs above listed. However at the end of the treatment (XII session) group A (treated with medical ozone) has shown a greater reduction of the subjective symptomatology pre-treatment than the control group B (treated with medical oxygen). Group A often reached 100% of the symptomatological reduction and this reduction was observed in the average of 20-30% higher in comparison with group B.
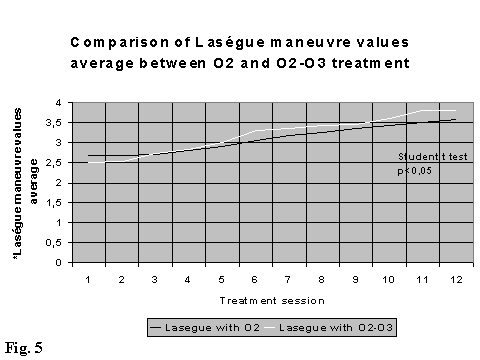
There is a statistical evidence (p < 0,001 Students t test for two samples matched by average), of a difference in evolution (time and intensity) of some clinical parameters (sciatic and low back pain, paraesthesia and Lasegue manoeuvre) between the two treated groups. For this reasons we report the only results in the follow up at three and six months regarding the group A (treated with medical ozone) (Fig. 2, 3, 4, 5).
DISCUSSION
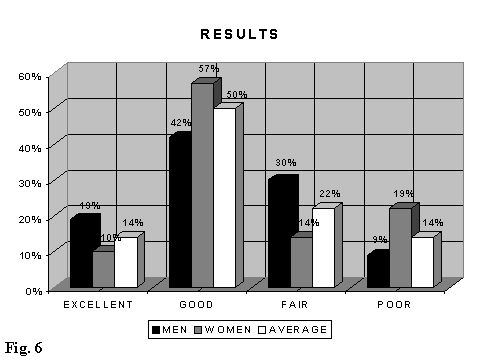
From our clinical series arises how the group A (treated with medical ozone) has shown the most significant improvement. The 14% of the patients (10% women and 19% men) have evidenced a clinical healing or an excellent result and the 72% a good or fair result, so that a positive result was obtained in 86% of the treated patients (Fig. 6).
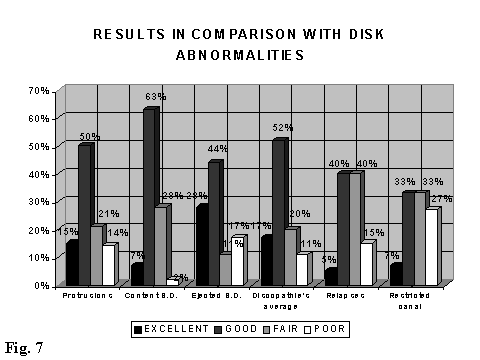
Regarding to the type of disk abnormalities and degree of improvement, we observed 28% of clinical healing or excellent results in the extruded herniation. This percentage decreases down to 15% in the disk protrusions and 7% in the contained herniations. Good or fair results has been found in 63% of contained herniations, in 50% of disk protrusions, in 44% of extruded herniations and in only 40% of recurrences of disk herniations. The poorer results have been observed in patients where the herniated disk occurred with a documented asimptomatic spinal canal stenosis (Fig. 7).
REFERENCES
Prof. GAETANO TORRI
ISTITUTO DI CLINICA ORTOPEDICA
DELL'UNIVERSITA' DEGLI STUDI DI MILANO
OSPEDALE C.T.O.